Lipedema patients experience pain and discomfort, intertwining physical and psychological issues, increasing feelings of isolation and self-blame.
Table of Contents
The key difference between lipedema and lymphedema is the cause: Lipedema is a fat disorder causing symmetrical fat accumulation in the limbs, while lymphedema is a lymphatic disorder causing fluid buildup (swelling). Lipedema affects mainly women and spares the hands and feet, while lymphedema can affect anyone and often includes the extremities. Here's a detailed comparison to help you understand which condition you may have and what treatments are available.
Lipedema and lymphedema are distinct medical and skin conditions, although they can appear quite similar, often presenting as skin dimpling and uneven, bumpy skin texture.
Adding to the confusion are the similar-sounding conditions: "lipedema" and "lymphedema." That, plus 15-17% of patients with lymphedema ALSO have lipedema, making distinguishing between the two even more challenging [1].
Recognising the symptoms of lipedema and lymphedema is the first step toward an accurate diagnosis and appropriate treatment.
Quick Comparison Table: Lipedema, & Lymphedema
| Lipedema | Lymphedema | |
|---|---|---|
| Definition | Painful fat disease with high output lymphatic failure | Localised subcutaneous tissue swelling |
| Occurrence | In females only | Males and females alike |
| Causes | • Genetic • Hormones • Inflammation • Fibrosis • Fluid build-up in tissues |
• Genetic defect • Cancer Treatment • Infection • Lymphatic system injury • Disrupted lymphatic system • Health conditions |
| Limbs affected | Both limbs affected by cuffs, including the arms and shoulders | One limb affected |
| Symptoms | • Pain and tenderness • Symmetrical swelling • Easy bruising • Heaviness in the affected area • Unusual or sudden fatigue • Reduced range of movement • Irregular fat distribution • Skin Changes |
• Pain and tenderness • Swelling in affected area, including fingers/toes • Heaviness and tightness in the affected area • Unusual or sudden fatigue • Reduced range of movement • Infections • Skin Changes |
| Skin | Tender to the touch | Thickened skin |
| Would a compression garment improve the appearance? | ✓ | X |
| Medical condition | ✓ | ✓ |
| Danger to health | • Immobility • Disability due to impaired daily activities • Orthopaedic changes |
• Immobility • Disability due to impaired daily activities • Recurring infection • Increased risk of cancer • May lead to other health or skin problems |
| Diagnosis | • Physical examination • Medical history • Ultrasound |
• Physical examination • Medical history • Ultrasound • NIRF lymphatic imaging • CT scans • Lymphoscintigraphy • MRI scans |
| Treatment | • Manual lymphatic drainage • Exercise • Compression garment • Lipedema Surgery with Liposuction |
• Manual lymphatic drainage • Exercise • Lymphedema Surgery |
What is Lipedema?
Lipedema is a chronic medical condition that affects about 11% of females.
It involves an abnormal accumulation of adipose tissue, usually affecting the legs and arms.
Those with lipedema may bruise easily, and the affected areas are usually painful to the touch.
Unfortunately, lipedema does not respond to diet and exercise.
It is often triggered or worsened by hormonal changes such as puberty, pregnancy, menopause, or even breastfeeding.
Lipedema stages and types

Stages of lipedema
| Stages | Lipedema description |
|---|---|
| Stage I | Skin looks smooth but feels pea-like |
| Stage II | More lipedema tissue, causing skin dimpling and larger nodules. Arms may show sagging tissue and a noticeable cuff around the wrists |
| Stage III | The lipedema tissue is thicker with many large nodules and hanging lobes of tissue. Patients (e) and (f) have lipedema, obesity and lipo-lymphedema. |
Note: A tissue cuff around the ankles or wrists can appear in all stages.
Type of lipedema
Types I to V describe the locations of lipedema tissue.
| Type | Locations of lipedema tissue |
|---|---|
| Type I | Around hips and buttocks |
| Type II | From under belly to knees |
| Type III | From under belly to ankles |
| Type IV | In arms |
| Type V | In lower legs (not shown) |
What is Lymphedema?
Lymphedema is the buildup of lymphatic fluid, unlike lipedema, which is characterised by fat accumulation.
Lymphedema can be either hereditary or acquired, such as from surgery or cancer treatment.
It typically affects only one limb, including hands and feet.
The key diagnostic indicator for lymphedema is the positive Stemmer's sign.
This condition cannot be addressed via surgery but can be effectively managed with compression and manual lymphatic drainage therapy.
Lymphedema Grades & Stages

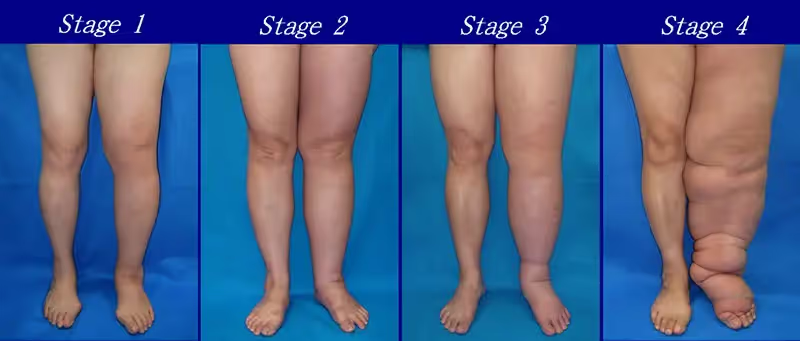
Stage 1 lymphedema: Swelling occurs during the day but subsides overnight when lying flat. The affected area may indent when pressed but may return to normal by morning. Treatment isn't usually needed.
Stage 2 lymphedema: Swelling does not go away overnight and requires management. The tissue becomes soft and bouncy rather than indented when pressed. This stage shows signs of limb hardening.
Stage 3 lymphedema: Swelling is permanent, and the affected area becomes larger and harder. Some people consider surgery to remove excess tissue, but it can be risky and might worsen lymphedema.
Stage 4 lymphedema: The affected limb becomes noticeably larger with bumps or lumps on the skin.
Can You Have Both?
Unfortunately, yes, you can.
Advanced lipedema can be accompanied by secondary lymphedema. It's when lipedema affects the lymphatic system, putting pressure on the lymphatic vessels, impeding their function, and leading to the accumulation and swelling of lymph fluid.
This combination of conditions is termed lipo-lymphedema, in which the systems of both conditions coexist and overlap.
This may complicate the diagnosis and the development of an accurate treatment plan.
Self-assessment on Lipedema & Lymphedema
How to self-check lipedema: Pinch test
How to do: Gently pinch the affected area and pay attention to any feeling of pain or if there's a difference in texture compared to other places. Pain or unusual texture could suggest lipedema.
Limitation: Not fully reliable, as overlapping conditions can affect results.
Red flag: Pain, tenderness, swelling, or limb heaviness impacting mobility
How to self-check lymphedema: The Stemmer's Sign test
How to do: The Stemmer's Sign test assesses the ability to pinch and lift the skin, especially at the bottom of the second toe or the middle finger.
If you can lift the skin easily, it is unlikely to be lymphedema (negative sign).
If it's a challenge, it might be lymphedema (positive sign).
Limitation: This test can give false positives and negatives, and it can't differentiate lymphedema from other conditions.
Red flag: Signs of infection (redness, warmth, pain, fever), worsening swelling, pain, or difficulty moving the affected area
Main Difference to pay attention to during self-check
| Main observation | Lipedema | Lymphedema |
|---|---|---|
| Symmetry check | Bilateral | Unilateral |
| When symptoms started | Often at puberty/pregnancy | Immediately after damage to the lymph system |
| Pain assessment | ✓ | X |
Importance of professional diagnosis
Professional diagnosis ensures that patients get the right treatment.
Therefore, receiving an accurate identification of whether they have lipedema, lymphedema, or a combination of both can improve their quality of life.
Treatment Comparison for Lipedema & Lymphedema
Lipedema Treatment:
- Liposuction (Scientifically proven to remove the diseased fat)
- MLD therapy (Supports lymphatic function)
- Compression garments
- Anti-inflammatory diet
Lymphedema Treatment:
- Complete Decongestive Therapy
- MLD therapy (Primary treatment)
- Compression bandaging/garments
- Exercise
- Surgery only for advanced cases (Lymph node transfer)
"Women with lipedema live with unbearable pain and invisible symptoms. We need to raise awareness of lipedema in Singapore so that women affected by this chronic medical condition can receive the necessary care. Lipedema is not just about appearance; it's also about health, mobility, and quality of life. Left untreated, it can worsen symptoms, including lymphedema and joint problems. That's why it's so crucial for patients to seek the right doctor — one with the experience, skill, and understanding to treat this complex condition effectively," shares Dr Ivan Puah, an MOH-accredited liposuction doctor who has successfully diagnosed and treated many patients with lipedema.
FAQ
What is the difference between lipedema and lymphedema?
Lipedema and lymphedema are conditions that affect the body's lymphatic system, but they are vastly different.
Lipedema is characterised by an abnormal accumulation of fat, while lymphedema occurs when the lymphatic system is blocked or damaged.
Can lipedema turn into lymphedema?
Those with lipedema can develop lymphedema.
The diseased fat in lipedema can put pressure on lymphatic vessels, potentially leading to lymph fluid buildup and resulting in lymphedema.
How can I visually identify whether I have lipedema or lymphedema?
Lipedema occurs in both legs or arms with a cuff on the ankle and wrist, whereas lymphedema often starts in the feet or hands.
What is the Stemmer's sign test?
The Stemmer's sign test is a clinical test used to help diagnose lymphedema.
A negative Stemmer's sign indicates no lymphedema present, meaning there is no fibrosis and subcutaneous thickening present.
Can liposuction treat lymphedema?
Liposuction is primarily used to treat lipedema. Lymphedema will require a different treatment and solution.
Why doesn't diet help lipedema?
Diet alone does not help reduce lipedema symptoms, as this medical condition is not caused by weight gain or caloric intake.
Is lipedema the same as being overweight?
While those with lipedema may typically have a higher BMI due to abnormal fat accumulation, lipedema differs from general obesity.
Who diagnoses lipedema in Singapore?
In Singapore, lipedema is typically diagnosed by medical doctors such as Dr Ivan Puah, who has experience in lipedema and its management.
LEARN MORE ABOUT LIPEDEMA SURGERY
Lipedema, lymphedema, and cellulite may appear similar, but they are distinct medical and skin conditions. Learn the difference for an accurate diagnosis.
Reference
- Warren Peled A, Kappos EA. Lipedema: diagnostic and management challenges. Int J Womens Health. 2016 Aug 11;8:389-95. doi: 10.2147/IJWH.S106227. PMID: 27570465; PMCID: PMC4986968.
- Figure 1: Herbst KL, Kahn LA, Iker E, Ehrlich C, Wright T, McHutchison L, Schwartz J, Sleigh M, Donahue PM, Lisson KH, Faris T, Miller J, Lontok E, Schwartz MS, Dean SM, Bartholomew JR, Armour P, Correa-Perez M, Pennings N, Wallace EL, Larson E. Standard of care for lipedema in the United States. Phlebology. 2021 Dec;36(10):779-796. doi: 10.1177/02683555211015887. Epub 2021 May 28. PMID: 34049453; PMCID: PMC8652358.
- Figure 2 & 3: Principles and Practice of Lymphedema Surgery. Cheng MH, Chang DW, Patel KM (Editors). Elsevier Inc, Oxford, United Kingdom. ISBN 978-0-323-29897-1. July 2015.
No reference