Recovery varies from person to person. Follow post-operative instructions, stay hydrated, care for wounds, wear compression garments & attend follow-ups.
Table of Contents
Common lipedema symptoms include disproportionately large legs compared to your upper body, pain and tenderness when legs are touched, easy bruising, and fat that doesn't respond to diet or exercise. Lipedema progresses through 3 stages, from small nodules under smooth skin (Stage 1) to large fat masses causing limb deformity (Stage 3).
Lipedema is an abnormal fat build-up medical condition that usually affects women.
It is characterised by the uneven distribution and disproportionate accumulation of fat and its supporting connective tissues.
The areas most commonly affected include the legs, arms, and buttocks, causing an uneven appearance compared to the other parts of the body.
10 Key Lipedema Symptoms

Specific symptoms of lipedema in the arms and legs
The 3 Stages of Lipedema
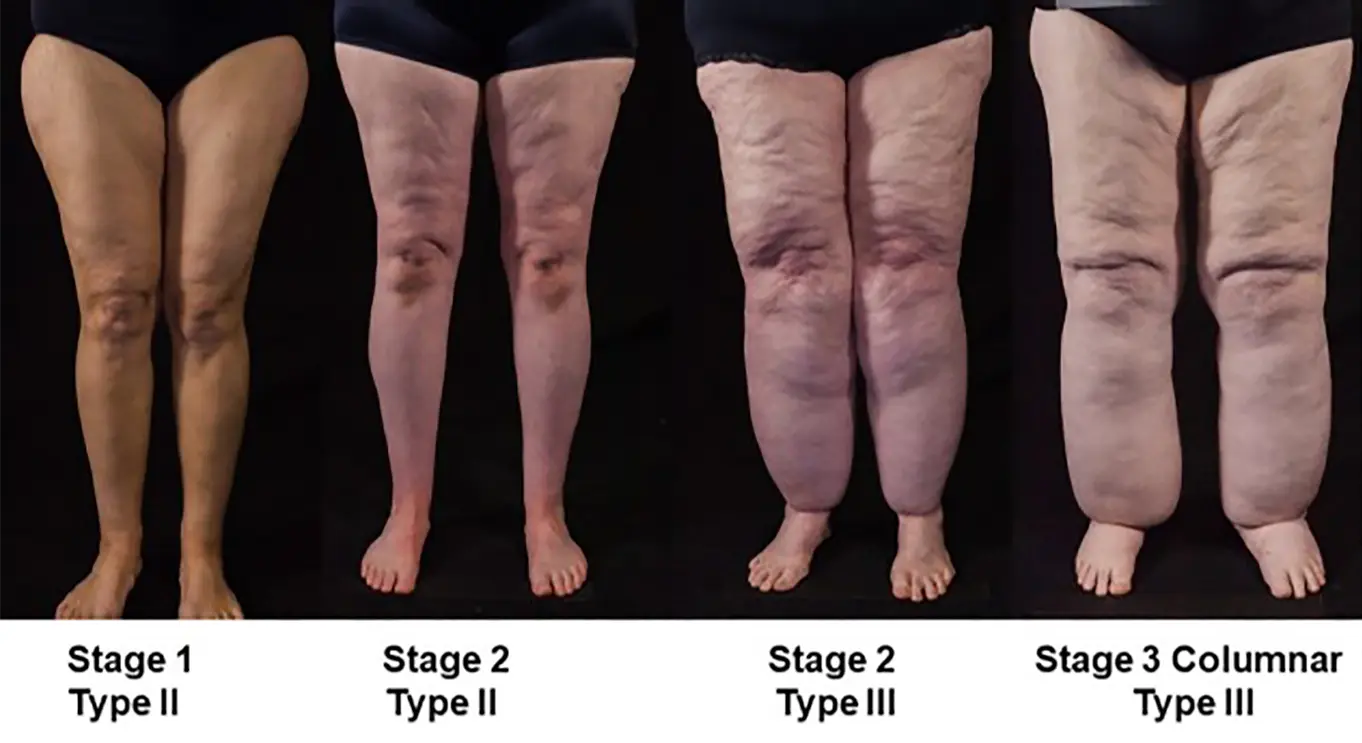
Stage 1:
- Skin surface: Normal, smooth
- Fat texture: Small nodules felt under skin
- Symptoms: Often mild, may be dismissed as 'normal'
Stage 2:
- Skin surface: Irregular, "orange peel" texture
- Fat texture: Larger nodules, induration
- Symptoms: More noticeable pain and swelling
Stage 3:
- Skin surface: Large folds, lobular deformity
- Fat texture: Large fatty masses
- Symptoms: Significant pain, mobility limitation
The 5 Types of Lipedema

Type I: Buttocks and hips (saddlebags)
Type II: Buttocks, hips, and thighs
Type III: Thighs, calves, and ankles
Type IV: Arms (with or without legs)
Type V: Lower legs only (calves, ankles)
Checking for lipedema at home with the pinch test
The only way to self-assess lipedema is through a pinch test.
The pinch test for lipedema involves gently pinching the affected area.
The goal of the pinch test is to assess the skin texture, pain response, and how the tissue feels.
During the pinch test, if the affected area has any pain or feels different in texture compared to other areas of your body, you may be suffering from lipedema.
However, the pinch test should NOT be regarded as a definitive diagnosis.
Lipedema Self-Assessment Checklist
For each question, check the box if it applies to you.
Scoring System
0 - 3 Checks: Low Likelihood of Lipedema
Symptoms may be related to typical weight gain, lymphedema, or venous insufficiency.
4 - 7 Checks: Possible Lipedema
It is recommended to consult a doctor who is experienced in diagnosing and managing lipedema, such as Dr Ivan Puah, for a formal diagnosis.
8+ Checks: High Probability of Lipedema
A medical assessment and investigation is strongly advised to manage symptoms and prevent progression.
FAQ on lipedema in Singapore
What are the early signs of lipedema in the arms and legs?
Lipedema often begins subtly, and recognising the early signs can make a significant difference in managing the condition effectively.
In the arms, early signs may include:
- A disproportionate increase in arm circumference, often stopping abruptly at the wrists
- Pain or tenderness, even with light touch or pressure
- Easy bruising without a known cause
- A sensation of heaviness or fullness in the upper arms
- The hands themselves typically remain unaffected, creating a distinct "cuff" at the wrist
In the legs, which are most commonly affected first, early signs may include:
- Symmetrical swelling in both legs, from the hips down to the ankles
- A "spongy" or nodular texture when pressing on the skin
- Cool skin temperature in the affected areas compared to the rest of the body
- Easy bruising, particularly on the thighs and calves
- A noticeable disproportion where the upper body remains slim while the lower body appears fuller
- The feet are usually spared, forming a characteristic "ankle cuff" or ring of tissue just above the ankle
If you notice these patterns, especially the combination of pain, easy bruising, and disproportionate fat distribution, it may be time to speak with a doctor experienced in lipedema.
At what age does lipedema start?
Lipedema most commonly begins or becomes noticeable during periods of significant hormonal change. For many women, early symptoms can appear:
- During puberty, often in the teenage years
- During or after pregnancy
- Around the time of menopause
While lipedema is a chronic and progressive condition, early recognition and intervention can help slow its progression and preserve mobility and quality of life.
Can men get lipedema?
Worldwide, approximately 0.2% of men may develop this condition.
The presentation in men is similar to that in women: symmetrical fat accumulation in the limbs that is painful, tender to the touch, and resistant to traditional weight loss methods.
How to self-care for lipedema at home?
While professional medical guidance is crucial for managing lipedema, there are several things you can do at home to support your overall well-being and complement your treatment plan:
- Move your body gently: Focus on enhancing blood and lymphatic circulation through low-impact exercises. Activities like walking, swimming, cycling, or gentle yoga can help maintain mobility without stressing your joints. The key is consistency, not intensity.
- Wear your compression garments regularly: If your doctor has prescribed medical-grade compression wear, wearing it consistently helps manage swelling, provides support, and can significantly reduce discomfort throughout the day.
- Adopt an anti-inflammatory approach to eating: While diet alone cannot remove lipedema fat, reducing inflammation can ease symptoms. Focus on whole, unprocessed foods and limit:
- Processed foods and takeaways
- Sugary drinks and snacks
- Refined carbohydrates like white bread and pastries
- Unhealthy fats are found in deep-fried foods
- Explore manual lymphatic drainage (MLD) massage: Regular MLD massage performed by a trained therapist can support your lymphatic system, helping to move excess fluid, reduce swelling, and promote a sense of lightness in the affected limbs.
When should you seek urgent help for lipedema?
While lipedema itself is a chronic condition, certain symptoms may indicate a complication that requires immediate medical attention.
Please visit the A&E or seek urgent care if you experience:
- Signs of cellulitis, a bacterial skin infection that can occur in advanced lipedema due to compromised lymphatic function
- Sudden redness and warmth in the swollen limbs
- Skin that becomes tender, hot, or painful to touch
- Fever or flu-like symptoms that accompany these changes.
- A general feeling of being unwell without a clear cause
These symptoms may signal a serious bacterial infection that requires prompt medical attention.
How is lipedema diagnosed?
A thorough lipedema diagnosis involves a comprehensive clinical assessment by an experienced physician. At Amaris B. Clinic, this includes:
- Visual inspection: Assessing for symmetrical fat enlargement, disproportionate body shape, and skin changes such as easy bruising or visible veins
- Palpation: Feeling the tissue for characteristic texture changes, nodules, sponginess, or fibrosis, and noting tenderness
- Negative Stemmer's sign test: Confirming that the hands and feet are unaffected, which helps differentiate lipedema from lymphedema
- Detailed medical history: Discussing symptom onset, family history, hormonal milestones, and how your body has responded to diet and exercise
There is no single blood test or scan that diagnoses lipedema. Imaging may be used to rule out other conditions, but the diagnosis remains clinical, based on what the doctor sees, feels, and hears from you.
Dr Ivan Puah brings years of experience to this diagnostic process, having assessed and treated lipedema cases in Singapore.
What triggers lipedema progression?
Lipedema progression is often linked to major hormonal shifts in a woman's life, including:
- Puberty
- Pregnancy
- Menopause
Significant weight gain can also accelerate the condition, as can a genetic predisposition.
Can lipedema get worse over time?
Lipedema is a progressive condition. According to The International Lipedema Association (ILA), the rate of progression varies significantly between individuals.
The condition remains relatively stable for decades for others, but for some, it may rapidly worsen, usually caused by:
- hormonal changes
- weight gain
- uncontrolled inflammation
Progression can be slowed with appropriate management, including conservative measures and, when indicated, surgical intervention.
What happens if lipedema is left untreated?
Lipedema is a progressive condition; without appropriate intervention, it typically worsens over time, leading to a cascade of physical and emotional challenges.
When left unmanaged, lipedema advances through stages. The pathological fat cells continue to accumulate, placing increasing pressure on the lymphatic system. Over time, this can lead to:
- Escalating pain: The pain can progress from tenderness/sensitivity to debilitating pain that affects your sleep and daily activities.
- Reduced mobility: As limb volume increases and pain intensifies, walking, climbing stairs, and even standing for extended periods become difficult. This creates a vicious cycle where reduced movement leads to further deconditioning, weight gain, and worsening symptoms.
- Skin changes: The skin may lose elasticity, develop fibrotic nodules (hardened areas), or become prone to infections.
- Lipo-lymphedema: Eventually, the overwhelmed lymphatic system begins to fail, leading to fluid retention on top of the existing fat. This combined condition, lipedema plus lymphedema—, s more complex to manage and carries a higher risk of complications such as cellulitis.
- Joint damage: The sheer weight and pressure of enlarged limbs place strain on knees, hips, and ankles, potentially contributing to osteoarthritis and chronic joint pain.
Early intervention matters. The goal of treating lipedema is not merely cosmetic; it is to stop progression, relieve pain, restore mobility, and improve quality of life.
Progression can be slowed with appropriate management, including conservative measures and, when indicated, surgical intervention.
What happens if lipedema is left untreated?
Lipedema is a progressive condition; without appropriate intervention, it typically worsens over time, leading to a cascade of physical and emotional challenges.
When left unmanaged, lipedema advances through stages. The pathological fat cells continue to accumulate, placing increasing pressure on the lymphatic system. Over time, this can lead to:
- Escalating pain: The pain can progress from tenderness/sensitivity to debilitating pain that affects your sleep and daily activities.
- Reduced mobility: As limb volume increases and pain intensifies, walking, climbing stairs, and even standing for extended periods become difficult. This creates a vicious cycle where reduced movement leads to further deconditioning, weight gain, and worsening symptoms.
- Skin changes: The skin may lose elasticity, develop fibrotic nodules (hardened areas), or become prone to infections.
- Lipo-lymphedema: Eventually, the overwhelmed lymphatic system begins to fail, leading to fluid retention on top of the existing fat. This combined condition, lipedema plus lymphedema—, s more complex to manage and carries a higher risk of complications such as cellulitis.
- Joint damage: The sheer weight and pressure of enlarged limbs place strain on knees, hips, and ankles, potentially contributing to osteoarthritis and chronic joint pain.
Early intervention matters. The goal of treating lipedema is not merely cosmetic; it is to stop progression, relieve pain, restore mobility, and improve quality of life.